Table of Contents
ToggleLiving with wet macular degeneration: Treatment options and lifestyle tips

Wet macular degeneration, also known as neovascular age-related macular degeneration (AMD), is a chronic eye condition that affects the macula—the central part of the retina responsible for sharp, detailed vision. Unlike the slower progression of dry AMD, wet AMD can lead to rapid vision loss if not treated promptly. While the diagnosis may feel overwhelming, advances in treatment and simple lifestyle adjustments can help patients maintain independence and a good quality of life.
In this blog, we will explore available treatment options and practical lifestyle tips for living with wet macular degeneration.
Understanding Wet Macular Degeneration
Wet AMD occurs when abnormal blood vessels grow under the retina and leak fluid or blood, leading to inflammation and, if left untreated, scarring of the macula. This distorts central vision, making tasks such as reading, recognising faces, or driving difficult.
Key symptoms include:
- Blurred or distorted central vision
- Straight lines appearing wavy or bent
- Dark or empty spots in the centre of vision
- Difficulty recognising faces
Early detection and timely treatment are essential to slow progression and preserve as much vision as possible.
Treatment options for wet macular degeneration
Although wet AMD cannot be cured, several treatments are available to control disease progression and improve vision outcomes.
1. Anti-VEGF Injections
The most common treatment involves anti-vascular endothelial growth factor (anti-VEGF) medications, which block abnormal blood vessel growth.
- Benefits: Can stabilise or improve vision in many patients.
2. Photodynamic Therapy (PDT)
A light-sensitive drug is injected into the bloodstream and then activated by a laser to destroy abnormal blood vessels in the eye.
- Best suited for: Patients with specific types of wet AMD.
- Limitations: Not as widely used today due to the effectiveness of anti-VEGF therapy.
3. Laser photocoagulation
A high-energy laser is used to seal abnormal blood vessels.
- Best suited for: Certain cases where abnormal vessels are not in the center of the macula.
- Limitation: May cause damage to surrounding retinal tissue and vision.
4. Emerging treatments
- Long-acting anti-VEGF implants: Provide sustained medication release, reducing injection frequency.
- Gene therapy and new biologics: Currently under clinical trials, offering hope for future treatment advances.
Lifestyle tips for living with wet macular degeneration
While medical treatment manages the condition, daily habits and environmental adjustments play a big role in maintaining independence and quality of life.
1. Nutrition and Diet
While medical treatment manages the condition, daily habits and environmental adjustments play a big role in maintaining independence and quality of life.

- Follow an eye-healthy diet rich in leafy greens, colourful fruits, and omega-3 fatty acids.
- Consider AREDS2 supplements (containing vitamins C, E, zinc, lutein, and zeaxanthin) if recommended by your doctor.
- Limit smoking and alcohol, as these can worsen AMD progression.
2. Protect Your Eyes

- Wear UV-protective sunglasses outdoors.
- Use good lighting at home to reduce eye strain while reading or doing tasks.
3. Home Adjustments
- Use magnifying lenses, large-print books, or digital devices with zoom functions.

- Install cool white, bright, adjustable lighting in key areas like the kitchen and study.
- Mark appliances with tactile or coloured stickers for easier use.
4. Technology and Low-Vision Aids
- Try screen readers, audiobooks, and voice-activated assistants.
- Use high-contrast settings on digital devices.
- Explore low-vision rehabilitation services that train you to adapt to vision changes.
5. Healthy Lifestyle Habits
- Exercise regularly to improve blood circulation and eye health.
- Manage underlying conditions such as high blood pressure, diabetes, and cholesterol.
- Get regular eye check-ups to monitor progression.
Coping emotionally and socially
Living with wet AMD can be emotionally challenging. Losing central vision affects independence and confidence, but the right support systems can make a big difference.
- Counselling and support groups can help manage frustration or anxiety.
- Family involvement is important—educate loved ones about your condition so they can provide assistance when needed.
- Stay socially active to avoid isolation, even if tasks take longer.
Conclusion
Wet macular degeneration may change the way you see the world, but it does not have to stop you from living a fulfilling life. With timely treatment, regular eye care, and lifestyle adjustments, many people successfully adapt and maintain independence. Embracing new tools, healthy habits, and emotional support can make daily living easier and more enjoyable.
If you notice sudden changes in your vision, seek immediate medical attention. Early diagnosis and proactive care are the keys to protecting your sight.
At Clarity Eye Surgeons, we offer advanced treatments and compassionate support to help you manage wet macular degeneration. Contact us today to book an appointment and take the first step towards protecting your vision.
Author Bio
Dr Parth Shah is a director and principal ophthalmologist at Clarity Eye Surgeons in Canberra, specialising in eye injections for retinal disease, cataract surgery & strabismus (eye muscle) surgery. With extensive training and experience, he is renowned for his expertise in the field. Dr Shah is dedicated not only to performing successful surgeries but also to patient education. His compassionate approach, combined with technical proficiency, has earned him the trust and gratitude of countless patients. He is a true advocate for eye health and a trusted name in the Canberra ophthalmology community.
FAQs
Yes, genetics can play a role. If you have a family history of AMD, your risk may be higher.
Dry AMD progresses slowly due to thinning and scarring of the macula, while wet AMD involves abnormal blood vessel growth that causes fluid to build at the macula, and can lead to rapid vision loss.
Yes, it often starts in one eye but may eventually affect both, making regular monitoring essential.
Vision loss can occur suddenly or progress rapidly over weeks to months if untreated.
Sometimes patients first have dry AMD, and sudden changes such as wavy lines or dark spots may indicate progression to the wet form.
This depends on the severity and legal vision requirements. An eye specialist can assess your ability to drive safely.
Coverage varies by country and provider; it is best to check with your insurer about eligibility. In Australia, if you are covered by medicare, this is rebatable on most anti-VEGF injections.
No, supplements cannot cure or stop wet AMD, but they may slow progression in certain cases when combined with medical treatment.
Other blogs related to Eye Conditions
Toric IOLs for astigmatism: Do they really reduce the need for glasses after cataract surgery?
Toric IOLs for astigmatism: Do they really reduce the need for glasses after cataract surgery? Cataract surgery today is not just about removing a cloudy
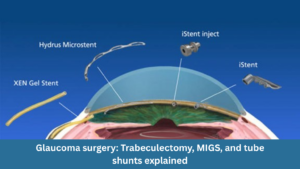
Glaucoma surgery: trabeculectomy, MIGS, and tube shunts explained
Glaucoma surgery: trabeculectomy, MIGS, and tube shunts explained Glaucoma is often called the “silent thief of sight” because it can gradually damage vision without obvious

Chalazion that won’t go away: What are your options?
Chalazion that won’t go away: What are your options? A small lump on your eyelid that simply refuses to disappear can be frustrating. While many
Blocked Tear Duct in Adults vs Children: What is the difference?
Blocked Tear Duct in Adults vs Children: What is the difference? A blocked tear duct, also known as nasolacrimal duct obstruction, is a common eye
Myopia (Short-sightedness) in Children — Causes, Progression, Prevention and Control
Myopia (Short-sightedness) in Children — Causes, Progression, Prevention and Control Myopia, commonly known as short-sightedness, is becoming increasingly common among children worldwide. Many parents first

Eye conditions in premature infants (e.g. ROP) — What parents should know
Eye conditions in premature infants (e.g. ROP) — What parents should know Premature infants face a range of medical challenges, and their eyes are no
Understanding thyroid eye disease: What you need to know
Understanding thyroid eye disease: What you need to know At Clarity Eye Surgeons in Canberra, our team of skilled ophthalmologists in Canberra brings years of
Surgery for thyroid eye disease: When is it needed?
Surgery for thyroid eye disease: When is it needed? At Clarity Eye Surgeons in Canberra, our team of experienced ophthalmologists, led by Dr Parth Shah,
Pterygium surgery: What to expect before, during, and after?
Pterygium surgery: What to expect before, during, and after? At Clarity Eye Surgeons in Canberra, patients receive expert care led by Dr Parth Shah, a
Living with thyroid eye disease: Treatment options explained
Living with thyroid eye disease: Treatment options explained At Clarity Eye Surgeons in Canberra, our team of highly qualified ophthalmologists has extensive experience diagnosing and
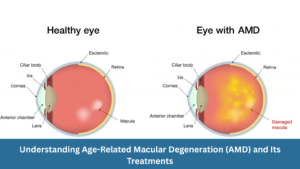
Understanding Age-Related Macular Degeneration (AMD) and Its Treatments
Understanding Age-Related Macular Degeneration (AMD) and Its Treatments At Clarity Eye Surgeons, we bring decades of ophthalmic expertise and advanced surgical experience to help Canberra
Diabetic eye disease: How to prevent vision loss?
Diabetic eye disease: How to prevent vision loss? What is diabetic eye disease? Diabetic eye disease refers to a group of eye conditions that can

Common vision problems in children and how to spot them early
Common vision problems in children and how to spot them early At Clarity Eye Surgeons in Canberra, our team of highly experienced paediatric ophthalmologists and

Double vision in children: What parents should know
Double vision in children: What parents should know Double vision, medically called diplopia, occurs when a child sees two images of a single object instead

Glaucoma: What it is, Symptoms, Causes, Types & Treatment
Glaucoma: What it is, Symptoms, Causes, Types & Treatment Glaucoma is often called the “silent thief of sight” because it can damage your vision gradually,

Living with wet macular degeneration: Treatment options and lifestyle tips
Living with wet macular degeneration: Treatment options and lifestyle tips Wet macular degeneration, also known as neovascular age-related macular degeneration (AMD), is a chronic eye

Retinal detachment: Early signs you should never ignore
Retinal detachment: Early signs you should never ignore Your eyes are extraordinary organs that allow you to experience the world in vivid colour, detail, and

Vitrectomy: What you need to know
Vitrectomy: What you need to know Vitrectomy is a specialised eye surgery performed to treat a range of disorders affecting the retina and vitreous —

Diabetes and your eyes: What you need to know
Diabetes and your eyes: What you need to know Diabetes is a chronic condition that affects how your body regulates blood sugar (glucose). While most

Nystagmus: Symptoms, Causes, and Treatments
Nystagmus: Symptoms, Causes, and Treatments Nystagmus is a condition in which the eyes make uncontrolled, repetitive movements. These movements can be slow or fast, side-to-side

What to know about blurry vision and diabetes?
What to know about blurry vision and diabetes? Blurry vision is a common and often early symptom of diabetes. If you or someone you know
Chalazion surgery: When is it necessary and What to expect
Chalazion surgery: When is it necessary and What to expect A chalazion is a common eyelid condition that can lead to discomfort, swelling, and cosmetic

Are prescription glasses effective for treating lazy eye?
Are prescription glasses effective for treating lazy eye? Lazy eye, also known as amblyopia, is a common vision problem in children, affecting a small percentage

Dry Eye Syndrome: Symptoms, Causes & Treatment
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

The Relationship Between Allergies and Eye Health in Children
Table of Contents Toggle 1. Symptoms of Allergies Affecting Eye Health in Children 2. Causes of Allergies Affecting Eye Health in Children 3. Potential Complications

Understanding Astigmatism: Symptoms, Causes, Diagnosis, Treatment Options & Prevention
Table of Contents Toggle What is Astigmatism? Sign & Symptoms of Astigmatism Causes of Astigmatism Types of Astigmatism Diagnosis Treatment Options for Astigmatism Astigmatism in
Understanding Retinal Detachment: Causes, Symptoms, Diagnosis and Treatment
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
