Table of Contents
ToggleGlaucoma surgery: trabeculectomy, MIGS, and tube shunts explained
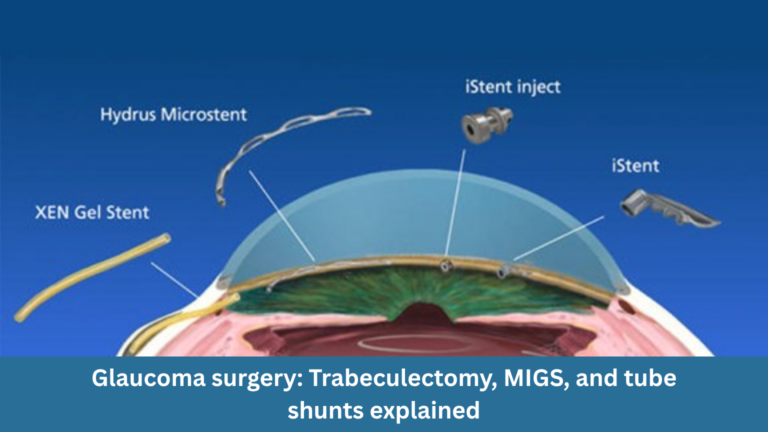
Glaucoma is often called the “silent thief of sight” because it can gradually damage vision without obvious symptoms. The primary goal of treatment is to lower intraocular pressure (IOP) to protect the optic nerve and preserve vision.
While eye drops and laser treatments are usually the first step, surgery becomes important when these options are no longer effective. Today, patients have several surgical options — ranging from traditional procedures to newer, minimally invasive techniques.
This guide explains the three main types of glaucoma surgery: trabeculectomy, MIGS, and tube shunt surgery — and how they differ.
Why is glaucoma surgery needed?
Glaucoma surgery is recommended when:
- Eye drops are not controlling eye pressure adequately.
- There is ongoing optic nerve damage.
- Medication side effects are difficult to tolerate.
- Advanced glaucoma is diagnosed, which requires lower target pressures.
All surgical treatments aim to improve the drainage of fluid (aqueous humour) from the eye, thereby lowering IOP.
1. Trabeculectomy: The gold standard
Trabeculectomy has been the traditional and most established glaucoma surgery for decades.
How it works
During the procedure:
- A small drainage flap is created in the white part of the eye. (sclera)
- Fluid drains into a reservoir (called a bleb) under the conjunctiva.
- This reduces intraocular pressure significantly.
When is it recommended?
Trabeculectomy is typically used for:
- Moderate to advanced glaucoma.
- Cases requiring very low eye pressure.
- Patients who have not responded to medications or laser.
Pros
- Highly effective at lowering eye pressure.
- Many years of patient data and well-studied outcomes.
Cons
- Higher risk of complications compared to newer procedures
- Longer recovery time
- Requires close post-operative monitoring
Despite newer options, trabeculectomy remains the gold standard surgery for glaucoma, particularly in advanced disease.
2. MIGS: Minimally Invasive Glaucoma Surgery
MIGS represents a newer category of procedures designed to be safer and less invasive.
How it works
MIGS procedures:
- Use microscopic instruments and tiny incisions.
- Improve natural drainage pathways or create new ones.
- Often involve tiny stents or implants.
These procedures enhance fluid outflow or reduce fluid production to lower pressure.
When is it recommended?
MIGS is best suited for:
- Mild to moderate glaucoma.
- Patients undergoing cataract surgery- as it can be done at the same time.
- Those wanting to reduce their dependence on eye drops.
Pros
- Safer with fewer complications.
- Faster recovery.
- Less disruption to eye tissues.
Cons
- May not lower pressure as much as traditional surgery.
- Not ideal for advanced glaucoma.
MIGS procedures are increasingly used earlier in the disease process, offering a balance between safety and effectiveness.
3. Tube shunts (glaucoma drainage devices)
Tube shunt surgery involves implanting a small device to help drain fluid from the eye.
How it works
- A tiny tube is inserted into the front of the eye.
- Fluid drains through the tube to a plate (reservoir) placed under the eyelid.
- The fluid is then absorbed by surrounding tissues.
When is it recommended?
Tube shunts are often used for:
- Complex or severe glaucoma.
- Cases where trabeculectomy has failed.
- Secondary glaucomas. (e.g. neovascular glaucoma)
Pros
- Effective in difficult or high-risk cases.
- Useful when other surgeries are unlikely to succeed.
Cons
- More invasive than MIGS.
- Risk of complications such as infection or tube-related issues.
Tube shunts provide an alternative drainage pathway and are particularly valuable in advanced or refractory glaucoma.
Which surgery is right for you?
There is no one-size-fits-all approach to glaucoma surgery. The best option depends on:
- The severity of your glaucoma.
- Your target eye pressure.
- Previous treatments or surgeries.
- Overall eye health.
For example:
- MIGS may be ideal if you have early glaucoma and are already having cataract surgery
- Trabeculectomy is often preferred when very low pressure is needed
- Tube shunts are typically reserved for more complex or previously treated cases
Conclusion
Advances in glaucoma surgery mean patients today have more options than ever before. From the proven effectiveness of trabeculectomy to the safety of MIGS and the versatility of tube shunts, treatment can be tailored to each individual.
The most important step is early diagnosis and ongoing monitoring, as timely intervention can help preserve vision for the long term.
If you have been diagnosed with glaucoma or are concerned about your eye pressure, a personalised assessment with an experienced ophthalmologist is essential. At Clarity Eye Surgeons, our team provides comprehensive glaucoma care — from advanced diagnostics to tailored surgical solutions. Book a consultation today to protect your vision and receive expert guidance on the most suitable treatment for your eyes.
Author bio
Dr Parth Shah is a director and principal ophthalmologist at Clarity Eye Surgeons in Canberra, specialising in paediatric ophthalmology. With extensive training and experience, he is renowned for his expertise in the field. Dr Shah is dedicated not only to performing successful surgeries but also to patient education. His compassionate approach, combined with technical proficiency, has earned him the trust and gratitude of countless patients. He is a true advocate for eye health and a trusted name in the Canberra ophthalmology community.
FAQs
No, glaucoma surgery does not cure glaucoma. It aims to control eye pressure and slow down vision loss, but ongoing monitoring is still essential.
Recovery time varies depending on the procedure. MIGS may take a few days to weeks, while trabeculectomy or tube shunt surgery may require several weeks to a few months for full recovery.
Some patients may still need eye drops after surgery, although often in reduced amounts. In some cases, drops may be stopped temporarily or completely.
Most glaucoma surgeries are performed under local anaesthesia, so you should not feel pain during the procedure. Mild discomfort or irritation can occur during recovery.
Glaucoma surgery is designed to preserve existing vision rather than improve it. Any vision already lost due to glaucoma cannot be restored.
Risks can include infection, bleeding, scarring, low eye pressure, or failure of the surgery over time. Your ophthalmologist will discuss these based on your individual case.
Success rates depend on the type of surgery and severity of glaucoma. Trabeculectomy generally has high success in lowering pressure, while MIGS has a strong safety profile with moderate pressure reduction
