Table of Contents
ToggleChalazion that won’t go away: What are your options?

A small lump on your eyelid that simply refuses to disappear can be frustrating. While many chalazia settle with simple home care, some linger for weeks or even months. If you are dealing with a chalazion that would not go away, understanding your options can help you decide what to do next.
What is a chalazion?
A chalazion is a slow-growing lump on the eyelid caused by a blocked meibomian (oil) gland. These glands normally produce oil that keeps your tears from evaporating too quickly. When the gland becomes blocked, the oil builds up and causes inflammation.
Unlike a stye, a chalazion is usually painless and not caused by an active infection. However, it can become tender if inflamed.
Why would not my chalazion go away?
Most chalazia improve within a few weeks with warm compresses and gentle eyelid hygiene. However, some persist due to:
- Ongoing gland blockage.
- Thickened oil secretions.
- Underlying blepharitis.
- Incomplete drainage.
- Recurrent inflammation.
In some cases, what appears to be a persistent chalazion may need medical assessment to rule out other eyelid conditions.
Home treatments you can try
If your chalazion has been present for less than a few weeks, conservative treatment is usually recommended first:
- Warm compresses for 10–15 minutes, 3–4 times daily.
- Gentle eyelid massage after warming.
- Maintaining good eyelid hygiene.
- Avoiding squeezing or popping the lump.
These measures help soften thickened oils and encourage natural drainage.
When should you see an eye specialist?
You should consider seeing an ophthalmologist if:
- The lump persists beyond 4–6 weeks.
- It becomes larger or more uncomfortable.
- It affects your vision.
- You experience repeated chalazia.
- The diagnosis is uncertain.
Persistent eyelid lumps should always be properly examined to confirm they are benign.
Medical treatment options
If home care does not resolve the chalazion, medical treatment may be recommended.
Steroid injection
A small corticosteroid injection into the lump can reduce inflammation and shrink the chalazion. This is a quick in-clinic procedure and may avoid the need for surgery.
Minor surgical removal
If the lump remains despite conservative measures, a simple minor procedure called incision and curettage may be performed. This involves:
- Local anaesthetic to numb the eyelid.
- A small incision on the inside of the eyelid.
- Removal of the blocked material.
The procedure is usually quick, and most patients return to normal activities within a day or two.
What if chalazia keeps coming back?
Recurrent chalazia may indicate underlying eyelid inflammation such as blepharitis or meibomian gland dysfunction. Long-term management may include:
- Ongoing lid hygiene.
- Prescription medications.
- Managing skin conditions such as rosacea.
- Lifestyle modifications.
Identifying and treating the root cause is key to preventing recurrence.
Is a persistent chalazion dangerous?
Most chalazia are harmless. However, a lump that does not respond to treatment, changes in appearance, or recurs in the same location should always be assessed. Rarely, other eyelid conditions can mimic a chalazion.
Early specialist evaluation provides peace of mind and appropriate management.
Conclusion
A chalazion that would not go away can be uncomfortable and concerning, but effective treatment options are available. From warm compresses and injections to minor surgical removal, the right approach depends on how long the lump has been present and how it responds to treatment.
If you have a persistent or recurrent eyelid lump, the experienced team at Clarity Eye Surgeons can provide a thorough assessment and tailored treatment plan. Don’t ignore a chalazion that lingers — book a consultation with Clarity Eye Surgeons today and take the next step towards clear, comfortable vision.
Author bio
Dr Parth Shah is a director and principal ophthalmologist at Clarity Eye Surgeons in Canberra, specialising in cataract surgery. With extensive training and experience, he is renowned for his expertise in the field. Dr Shah is dedicated not only to performing successful surgeries but also to patient education. His compassionate approach, combined with technical proficiency, has earned him the trust and gratitude of countless patients. He is a true advocate for eye health and a trusted name in the Canberra ophthalmology community.
FAQs
While many chalazia resolve within a few weeks, some can persist for months. Spontaneous resolution is still possible, but the likelihood decreases over time. If a lump has remained unchanged for several months, assessment by an ophthalmologist is recommended.
Contact lenses do not directly cause a chalazion, but wearing them while your eyelid is inflamed may increase irritation. It is often advisable to switch to glasses temporarily until the eyelid settles.
It is best to avoid eye makeup while you have an active chalazion. Makeup can block oil glands further and may introduce bacteria. Old or contaminated makeup should also be discarded to reduce the risk of recurrence.
Stress itself does not directly cause a chalazion, but it can weaken immune function and exacerbate underlying skin conditions such as rosacea or blepharitis, which may increase the risk.
In children, conservative treatment is usually tried first. However, if the chalazion is large, affects vision, or persists for an extended period, minor surgical removal may be recommended. In younger children, this may sometimes require treatment under general anaesthesia.
A diet low in omega-3 fatty acids may contribute to thicker gland secretions in some individuals. Increasing omega-3 intake through diet or supplements may support healthier meibomian gland function, particularly in people with recurrent episodes.
When performed correctly, incision and curettage is usually done from the inside of the eyelid, meaning visible scarring is uncommon. Healing is typically quick with minimal cosmetic impact.
A chalazion itself is not contagious and cannot spread. However, underlying eyelid conditions such as blepharitis can affect both eyes, increasing the risk of developing chalazia in either eyelid.
Other blogs related to Eye Conditions

Chalazion that won’t go away: What are your options?
Chalazion that won’t go away: What are your options? A small lump on your eyelid that simply refuses to disappear can be frustrating. While many
Blocked Tear Duct in Adults vs Children: What is the difference?
Blocked Tear Duct in Adults vs Children: What is the difference? A blocked tear duct, also known as nasolacrimal duct obstruction, is a common eye
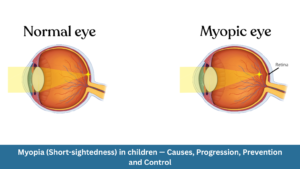
Myopia (Short-sightedness) in Children — Causes, Progression, Prevention and Control
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Eye conditions in premature infants (e.g. ROP) — What parents should know
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
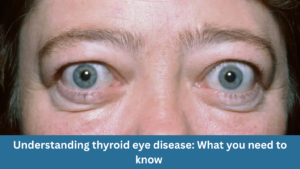
Understanding thyroid eye disease: What you need to know
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
Surgery for thyroid eye disease: When is it needed?
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
Pterygium surgery: What to expect before, during, and after?
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
Living with thyroid eye disease: Treatment options explained
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
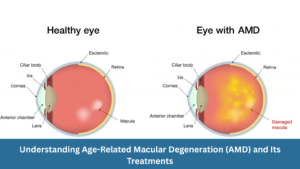
Understanding Age-Related Macular Degeneration (AMD) and Its Treatments
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
Diabetic eye disease: How to prevent vision loss?
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Common vision problems in children and how to spot them early
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Double vision in children: What parents should know
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Glaucoma: What it is, Symptoms, Causes, Types & Treatment
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Living with wet macular degeneration: Treatment options and lifestyle tips
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Retinal detachment: Early signs you should never ignore
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Vitrectomy: What you need to know
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Diabetes and your eyes: What you need to know
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Nystagmus: Symptoms, Causes, and Treatments
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

What to know about blurry vision and diabetes?
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
Chalazion surgery: When is it necessary and What to expect
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Are prescription glasses effective for treating lazy eye?
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Dry Eye Syndrome: Symptoms, Causes & Treatment
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

The Relationship Between Allergies and Eye Health in Children
Table of Contents Toggle 1. Symptoms of Allergies Affecting Eye Health in Children 2. Causes of Allergies Affecting Eye Health in Children 3. Potential Complications

Understanding Astigmatism: Symptoms, Causes, Diagnosis, Treatment Options & Prevention
Table of Contents Toggle What is Astigmatism? Sign & Symptoms of Astigmatism Causes of Astigmatism Types of Astigmatism Diagnosis Treatment Options for Astigmatism Astigmatism in
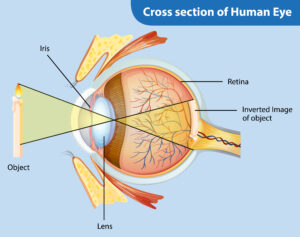
Understanding Retinal Detachment: Causes, Symptoms, Diagnosis and Treatment
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
