Table of Contents
ToggleBlocked Tear Duct in Adults vs Children: What is the difference?
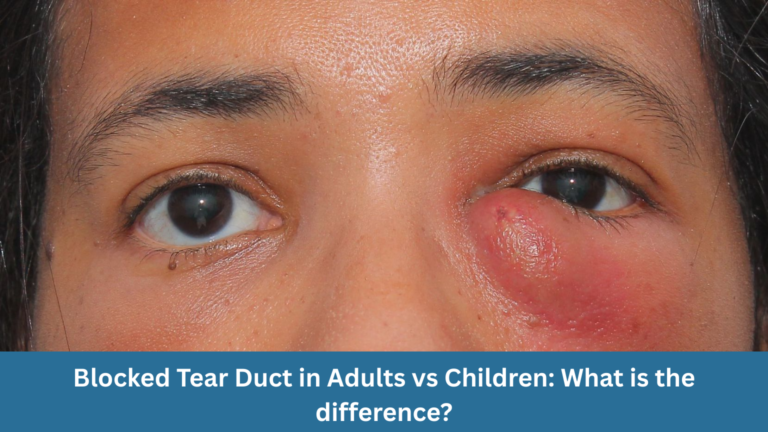
A blocked tear duct, also known as nasolacrimal duct obstruction, is a common eye condition that affects both babies and adults. While the symptom of watery eyes may look similar, the causes, risks and treatment options can be quite different.
Understanding these differences helps ensure the right care at the right time.
What is a blocked tear duct?
Tears normally drain from the eye through small openings in the eyelids into the tear duct, which carries them into the nose. When this drainage pathway becomes blocked, tears build up and overflow onto the face.
This can lead to:
- Constant watering of the eye.
- Sticky discharge.
- Recurrent eye infections.
- Redness or swelling near the inner corner of the eye.
Blocked tear duct in children
Blocked tear ducts are very common in newborns and infants. In most cases, the tear duct has not fully opened at birth.
Causes in children
- Incomplete development of the tear duct.
- Thin membrane remaining over the duct opening.
- Rarely, structural abnormalities.
Symptoms in children
- Persistent watery eye from birth.
- Sticky discharge, especially after sleep.
- Mild redness around the eyelids.
Treatment in children
The good news is that most cases resolve naturally within the first year of life.
Management may include:
- Gentle tear duct massage.
- Cleaning away discharge.
- Antibiotic drops if infection occurs.
If the blockage does not clear after 12 months of age, a simple probing procedure may be recommended.
Blocked tear duct in adults
In adults, a blocked tear duct is less likely to resolve on its own and may signal an underlying issue.
Causes in adults
- Age-related narrowing of the tear duct.
- Chronic sinus disease.
- Infection or inflammation.
- Injury or facial trauma.
- Previous nasal or sinus surgery.
- Rarely, a growth or tumour.
Symptoms in adults
- Constant watery eyes. (often worse outdoors or in wind)
- Recurrent painful infections. (dacryocystitis)
- Swelling near the inner corner of the eye.
- Mucus discharge.
Unlike in children, adult blockage is often progressive and may worsen over time.
Key differences between adults and children
Cause
- Children: Usually developmental and present from birth.
- Adults: Often due to narrowing, inflammation or other medical conditions.
Natural resolution
- Children: Frequently clears without surgery.
- Adults: Rarely resolves without treatment.
Infection risk
- Children: Usually mild and manageable.
- Adults: Higher risk of painful recurrent infections.
Treatment approach
- Children: Massage and monitoring first
- Adults: Surgery is often required for lasting relief.
Treatment options for adults
When symptoms persist or infections recur, a surgical procedure called dacryocystorhinostomy (DCR) may be recommended. This procedure creates a new drainage pathway for tears into the nose.
DCR can be performed externally or endoscopically through the nose, depending on the individual case. The success rate is generally high, and it significantly improves symptoms.
When to see an eye specialist?
You should seek specialist assessment if:
- Watery eyes persist for several weeks.
- There is pain, swelling or redness.
- Discharge becomes thick or yellow.
- Symptoms keep returning.
Early evaluation is especially important in adults to rule out more serious causes.
Conclusion
While blocked tear ducts in children are often temporary and harmless, in adults they are more likely to require medical or surgical treatment. The underlying causes, risk of complications and management strategies differ significantly between age groups.
If you or your child are experiencing persistent watery eyes or recurrent infections, professional assessment is essential. At Clarity Eye Surgeons, our experienced ophthalmic team provides comprehensive evaluation and advanced treatment for tear duct conditions in both adults and children.
Book a consultation with Clarity Eye Surgeons today to receive expert, personalised care and long-term relief.
Author bio
Dr Parth Shah is a director and principal ophthalmologist at Clarity Eye Surgeons in Canberra. With extensive training and experience, he is renowned for his expertise in the field. Dr Shah is dedicated not only to performing successful surgeries but also to patient education. His compassionate approach, combined with technical proficiency, has earned him the trust and gratitude of countless patients. He is a true advocate for eye health and a trusted name in the Canberra ophthalmology community.
FAQs
Yes. Excess tearing can temporarily blur vision because tears pool on the surface of the eye. However, once the tears are wiped away, vision usually clears. Persistent blurred vision should always be assessed by an eye specialist.
No, the blockage itself is not contagious. However, if there is an associated eye infection, the infection may spread through direct contact.
Allergies do not directly block the tear duct, but chronic inflammation from allergies may contribute to swelling around the drainage system, worsening watering symptoms.
An ophthalmologist may perform a clinical examination, tear drainage testing, or imaging studies if needed. In some cases, saline irrigation is used to check whether the duct is open.
In adults especially, untreated blockage can lead to recurrent infections, painful swelling, or abscess formation. Rarely, chronic obstruction may mask more serious underlying conditions.
Yes, although it is more common for only one eye to be affected. Bilateral blockage can occur, particularly in newborns or in adults with systemic or inflammatory conditions.
Other blogs related to Eye Conditions

Chalazion that won’t go away: What are your options?
Chalazion that won’t go away: What are your options? A small lump on your eyelid that simply refuses to disappear can be frustrating. While many
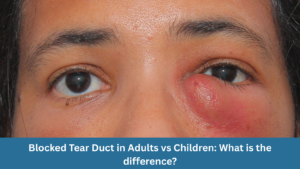
Blocked Tear Duct in Adults vs Children: What is the difference?
Blocked Tear Duct in Adults vs Children: What is the difference? A blocked tear duct, also known as nasolacrimal duct obstruction, is a common eye
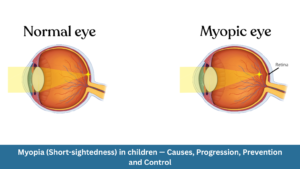
Myopia (Short-sightedness) in Children — Causes, Progression, Prevention and Control
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Eye conditions in premature infants (e.g. ROP) — What parents should know
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
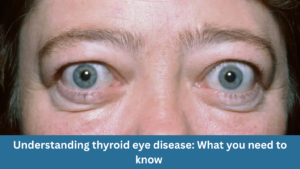
Understanding thyroid eye disease: What you need to know
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
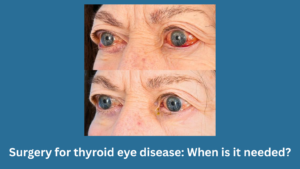
Surgery for thyroid eye disease: When is it needed?
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
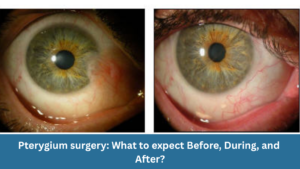
Pterygium surgery: What to expect before, during, and after?
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
Living with thyroid eye disease: Treatment options explained
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
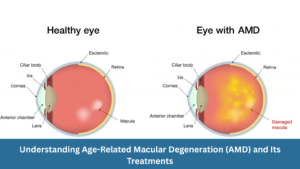
Understanding Age-Related Macular Degeneration (AMD) and Its Treatments
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
Diabetic eye disease: How to prevent vision loss?
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Common vision problems in children and how to spot them early
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Double vision in children: What parents should know
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Glaucoma: What it is, Symptoms, Causes, Types & Treatment
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Living with wet macular degeneration: Treatment options and lifestyle tips
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Retinal detachment: Early signs you should never ignore
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Vitrectomy: What you need to know
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Diabetes and your eyes: What you need to know
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Nystagmus: Symptoms, Causes, and Treatments
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

What to know about blurry vision and diabetes?
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
Chalazion surgery: When is it necessary and What to expect
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Are prescription glasses effective for treating lazy eye?
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

Dry Eye Syndrome: Symptoms, Causes & Treatment
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment

The Relationship Between Allergies and Eye Health in Children
Table of Contents Toggle 1. Symptoms of Allergies Affecting Eye Health in Children 2. Causes of Allergies Affecting Eye Health in Children 3. Potential Complications

Understanding Astigmatism: Symptoms, Causes, Diagnosis, Treatment Options & Prevention
Table of Contents Toggle What is Astigmatism? Sign & Symptoms of Astigmatism Causes of Astigmatism Types of Astigmatism Diagnosis Treatment Options for Astigmatism Astigmatism in
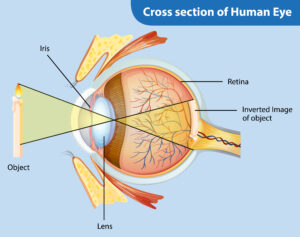
Understanding Retinal Detachment: Causes, Symptoms, Diagnosis and Treatment
Table of Contents Toggle What is Retinal Detachment? Causes of Retinal Detachment Symptoms of Retinal Detachment Diagnosis of retinal detachment Treatment Options for Retinal Detachment
