Table of Contents
ToggleEye injections in Elderly patients: Special considerations
At Clarity Eye Surgeons in Canberra, Dr Parth Shah has extensive experience in providing safe, effective eye injection treatments for elderly patients with complex retinal and macular conditions. With aging eyes often affected by multiple medical issues, anatomical changes and reduced resilience, eye injections in older adults require careful assessment, precise technique and compassionate patient-centred care.
Using advanced diagnostic imaging, evidence-based treatment protocols and a gentle, reassuring approach, Clarity Eye Surgeons ensure that elderly patients receive injections that are not only clinically effective but also comfortable and confidence-building. Even patients considered “high-risk” or anxious about injections elsewhere can feel reassured under expert care.
Understanding eye injections and why age matters
Eye injections, the most common being intravitreal injections, involve delivering medication directly into the vitreous cavity of the eye. This targeted approach allows high concentrations of medication to reach the retina and macula, where many age-related eye diseases occur.
In elderly patients, injections are most commonly used to treat conditions such as:
- Age-related macular degeneration. (AMD)
- Diabetic macular oedema.
- Retinal vein occlusion.
- Inflammatory retinal conditions.
Age plays a critical role in treatment planning because older eyes often have reduced healing capacity, co-existing eye diseases, and systemic medical conditions such as diabetes, hypertension or arthritis. These factors influence injection frequency, monitoring needs and overall safety.
How do eye injections differ in elderly patients?
Age-related anatomical and physiological changes
As we age, the eye undergoes natural changes that affect injection delivery and outcomes.
Key considerations include:
- Thinner, more fragile ocular tissues.
- Reduced tear production leading to dry eye.
- Increased risk of infection due to reduced immune response.
- Slower recovery from inflammation.
These changes make meticulous technique and post-injection care especially important in elderly patients.
Common eye conditions requiring injections in older adults
Age-related macular degeneration (AMD)
AMD is one of the leading causes of vision loss in Australians over the age of 60.
Special considerations in elderly patients:
- Treatment often requires long-term or lifelong injections.
- Vision may fluctuate, requiring close monitoring.
- Anxiety or fear of repeated injections is common.
How injections help?
Anti-VEGF injections can slow or halt vision loss, preserve central vision and maintain independence for daily activities such as reading and recognising faces.
Diabetic eye disease
Many elderly patients have long-standing diabetes, increasing the risk of retinal damage.
Special considerations:
- Blood sugar control affects treatment response.
- Healing may be slower.
- Co-existing cataracts or glaucoma may complicate care.
Eye injections help reduce retinal swelling and stabilise vision when combined with good systemic disease management.
Retinal vein occlusion
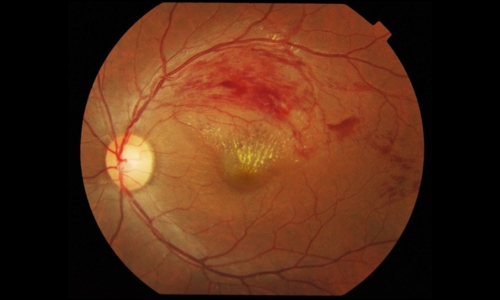
Blockages in retinal veins are more common with age and cardiovascular disease.
Special considerations:
- Monitoring blood pressure and vascular health.
- Regular imaging to assess treatment response.
- Gradual visual recovery rather than immediate improvement.
Managing anxiety and comfort in elderly patients
Fear of injections is common, particularly among older adults.
Supportive strategies include:
- Clear, step-by-step explanations in simple language.
- Allowing carers or family members to attend appointments.
- Using calming communication and reassurance during treatment.
- Minimising waiting times to reduce stress.
Most patients report that the injection itself is quick and far more comfortable than expected.
Expected treatment experience and recovery
During the injection
- Performed in a sterile clinic environment.
- No general anaesthetic required.
- The eye is numbed with drops.
- Injection takes only a few seconds.
- Total appointment time is usually 20–30 minutes.
Recovery timeline
- Same day: Mild irritation or gritty sensation.
- 24–48 hours: Vision settles, redness reduces.
- 1 week: Eye feels normal again for most patients.
- Ongoing: Regular follow-up and imaging as required.
Most elderly patients resume normal daily activities within a day.
Risks, considerations and safety in elderly patients
Eye injections are very safe when performed by experienced specialists, but age-related factors are carefully considered.
Possible risks include:
- Temporary discomfort or redness.
- Mild floaters after injection.
- Infection (very rare)
- Short-term pressure rises in the eye.
- Dry eye symptoms during healing.
Strict infection-control protocols significantly minimise risks.
Conclusion
Eye injections play a crucial role in preserving vision and independence for elderly patients with retinal and macular disease. While aging eyes require additional care and consideration, modern injection therapy is highly effective and well tolerated when delivered by experienced specialists.
At Clarity Eye Surgeons, elderly patients benefit from personalised treatment plans, advanced diagnostic technology and a compassionate approach that prioritises comfort, safety and long-term visual health. If you or a loved one require retinal injections and would like expert guidance, book a consultation today and take a proactive step towards protecting your vision.
Author bio
Dr Parth Shah is a director and principal ophthalmologist at Clarity Eye Surgeons in Canberra, specialising in eye injections. With extensive training and experience, he is renowned for his expertise in the field. Dr Shah is dedicated not only to performing successful surgeries but also to patient education. His compassionate approach, combined with technical proficiency, has earned him the trust and gratitude of countless patients. He is a true advocate for eye health and a trusted name in the Canberra ophthalmology community.
FAQs
The frequency varies depending on the condition, response to treatment, and imaging results. Some patients require monthly injections initially, while others move to less frequent maintenance schedules.
Yes. Most blood-thinning medications do not need to be stopped before eye injections, but your ophthalmologist will assess your medication list to ensure safe treatment.
Some patients experience temporary blurred vision after the injection, so driving is usually not recommended on the same day. Vision typically stabilises within 24 hours.
Yes. With appropriate communication, caregiver involvement, and gentle techniques, injections can be safely administered to patients with cognitive challenges.
In certain situations, same-day bilateral injections may be considered. This decision is based on safety protocols, patient preference, and clinical necessity.
Missing injections may allow disease activity to return and vision to decline. If an appointment is missed, patients should contact the clinic promptly to reschedule.
